Inequalities in health
On international women’s day one of the topics that MediPaCe would like to focus on are the inequalities in the way that people experience poor health: diseases, health-information, social reactions to disease, research-funding, health research, care and access. Our aim with this article is to provide an overview of some of the key themes as well as an introduction for anyone not familiar with the area.
Longtime gender biases are deeply rooted in many cultures. Such deeply embedded cultural bias is often one of the most difficult for each of us to see, and even harder to address. It’s a part of our social human nature for a group of people to try to return behaviours to the social norms for their culture. It is easier to perpetuate what is recognized as ‘okay’ and to question behaviours that differ from this ‘normal’, than it is to question whether ‘normal’ itself is the right action in the first place. This means that, in areas such as healthcare, all of us need to specifically analyse and collect data to understand what happening – sometimes from people who do not normally get their voices heard. We need to listen in a way that doesn’t normally occur to be able to hear what people are not normally getting to say.
Gender-inequalities are affected by many other, separate but widely acknowledged, factors that affect healthcare: different geographical locations, economic status, education and health-literacy, sociocultural factors, and policies. As a consequence of this, the issue of gender inequality is complex, with nearly all health conditions being experienced differently by the different genders.
Key knowledge gaps are highlighted in the diagram, with each discussed in more detail below.
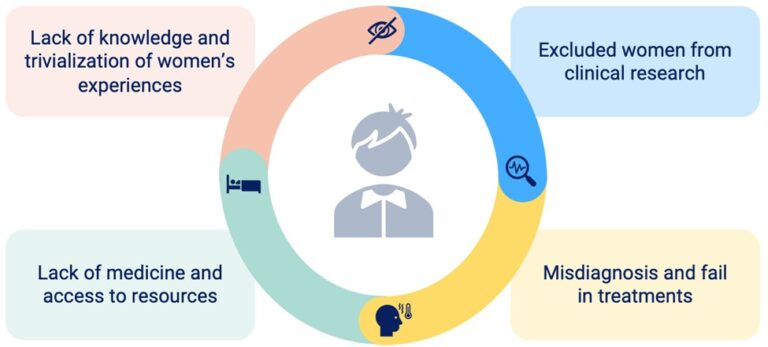
The lack of knowledge about sex-related differences and trivialization of women's complaints (women did not feel seen or heard)
For centuries, there was a perpetuated stereotype – if a woman complained about their health conditions, ‘female hysteria’ was a common medical diagnosis. Even though this is no longer the case, curiosity about female experience of disease and whether it is different from male experiences, has been understudied academically for so long that there are fewer available resources. This has resulted in a ‘tradition’ of women being, quite often non-purposefully but systemically, overlooked and under-represented in healthcare [1]. This difference in representation has caused a gender data-gap that has led to a lack of knowledge about conditions that primarily or predominantly affect women, or affect women differently. All of these have an impact on women’s health options, under- and over-diagnosis of certain conditions, individual self-confidence and, ultimately, patient well-being [2].
This is especially prevalent in tricky-to-measure conditions such as women reporting pain. Researchers have found that providers may not have worked with the patient when diagnosing conditions. In particular, patient’s perceived that their expertise in their own bodies and health was not respected, and they were not given tools and information to understand what is going on. In several cultures, if these interactions occur, women simply do not feel seen or heard and this can result in feelings of fear, guilt, and shame about asking questions and for clinical support [3].
A good example of this comes from our past when doctors have been confused by the higher mortality rate of women with cardiovascular disease (CVD) than that seen in men [4]. As men are at higher risk of experiencing CVD in the first place, this condition is considered by many to be a predominantly male problem. People commonly assumed that it was therefore females’ lack of knowledge about the symptoms of CVD in women that caused the gender gap in the treatment-of and death-rate from CVD. It seemed plausible that, without access to gender-specific knowledge about CVD, women would be hesitant to seek medical attention or would not report that they had experienced key heart-related symptoms. However, women’s accounts of their symptoms being dismissed have been backed up by academic studies and show that physicians administer far fewer diagnostic tests and treatments for CVD in women than men. The cause of this difference in mortality rate is therefore unlikely to be solved by more education for women alone, the bias itself also needs to be addressed [4].
The underrepresentation of women in health studies and clinical trials and the impact of data failure
The lack of knowledge caused by marginalizing women-specific health conditions or believing that women’s experiences are simply the same as men’s has resulted in a general underrepresentation of women and women-specific conditions in healthcare studies and clinical trials [2]. Research and data collection related to women’s health has shown to be underfunded [4]. Research into the treatment of health issues specific to women, such as pregnancy and menopause has traditionally not been prioritized within many health agendas where approximately 1% of healthcare research and innovation is invested in female-specific conditions beyond oncology [5]. Furthermore, standard data calculations and decisions may need to be modified for women but this research has never been undertaken and shared broadly enough to have a wide impact on clinical practice. For example, Lai, Pomfret and Verna (2022), report unconscious bias within liver transplant delivery. Women with liver cirrhosis waiting for a liver transplantation were less likely to receive a transplant and more likely to die than men in the same situation. The authors concluded that there was “undeniable presence of implicit bias within our health care system”. When researching the issues it was found that one of the factors involved in this disparity was the difference in body size and how this affected standard methods for estimating kidney function. The outputs of this standard calculation resulted in the underestimation of mortality risk due to renal dysfunction for women on the waiting list [6].
Misdiagnosis and poorer treatment outcomes
A lack of awareness among health care professionals about the importance of sex-specific differences in disease manifestation may result in either mis-diagnosis or late diagnosis [3]. In addition, gender-related differences in treatment response is an understudied area and may well be resulting in clinicians simply not having the right information to be able to plan a tailored treatment pathway optimally. Both of these can cause gender-related problems in diagnosis in the early stages and treatment.
Evidence suggests that a key knowledge-gap is the characterisation of symptoms and early-warning signs for conditions and how they differ between sexes. As a result, risk of misdiagnosis for a heart attack in women has been reported to be 50% higher than in men. This disparity in health outcome is compounded further by the fact that, in some cultures, women are less likely to be prescribed medicines to reduce their risk of suffering another heart attack. Where this occurred, women are more likely than men to die after a heart emergency [7].
In addition, women continue to experience 1.5 times more adverse effects to prescription medicines than men [8]. Medicine development has traditionally been designed around men’s physiology rather than that of women. There is simply insufficient research to be able to understand which of these are a consequence of a change in perception/experience of a similar side effect, or which are different characteristics of a side effect resulting from different physiology. Either way, in the real-world life, the consequences are very similar for the experience of women [6].
Lack of medicine and access to resources
All people have the equal right to have access to physical and mental health. Despite great progress in that regard, gender inequalities in healthcare are widely reported in clinical encounters, as physicians make assumptions about women’s health based on gender stereotypes about pain thresholds and patient credibility [9]. Data from several researchers has shown to identify the effects of gender inequalities and the principal social determinants of health, such as healthcare delivery at the levels of interpersonal relationships, teamwork and healthcare system design, access to financial resources, access to education, employment, working conditions, social protection and environment. [10], [11], [12]. Additionally, there are clear inequalities in health related to gender as well as to age, socioeconomic status and ethnicity of the cultures, and these factors are all interlinked. Poorer, migrant, older women suffer the worst health of all. There are further differences in health outcomes between ethnic groups, but for all groups ,poorer women have relatively low health outcomes [12].
As a result, even if we assume biases are unconscious and automatic, there are important actions which can be taken by policy makers nationally and locally, and by those within the health system strategies at the individual and the center level to be effective at reducing the influence of bias on the gender inequity.
Improving women’s health requires changes in many aspects that integrate women’s lifelong needs into health policies, health-in-all-policies approaches and intersectoral action. Engagement of women to ensure that they are at the center of these changes is a defining factor for success. Such programs should be established within and mandated by healthcare systems and may help to, over time, change the culture to promote gender equity in healthcare delivery.
We at MediPaCe are trying to increase the diversity and equity of access and support for all underrepresented patients and care partners when getting their voices heard in the medicines-development process. We acknowledge that there is more work to be done to ensure that patients are fairly represented in the research funding decisions, inputting into the next generation of medicines, and evaluation of patient-experience results.
If this is also something that you are interested in, please get in touch.

References:
World Health Organisation. Strategy on women’s health and wellbeing in the WHO European region.
www.mckinsey.com. Unlocking opportunities in women’s healthcare.
- Jianhua Wu, Chris P Gale, Marlous Hall, Tatendashe B Dondo, Elizabeth Metcalfe, Ged Oliver, Phil D Batin, Harry Hemingway, Adam Timmis, Robert M West. Impact of initial hospital diagnosis on mortality for acute myocardial infarction: A national cohort study.
- J. Bartley and R. B. Fillingim. Sex differences in pain: a brief review of clinical and experimental findings.
- Nicole C Woitowich, Annaliese Beery, Teresa Woodruff. Meta-Research: A 10-year follow-up study of sex inclusion in the biological sciences.
- Jessica Allen and Flavia Sesti. Health inequalities and women –addressing unmet needs.



